- +852 4750 3485
- info@mycancerinfo.org
Want to learn how liquid biopsy may help you choose suitable natural substances during your cancer journey?
Expert insights, latest research, and practical advice to empower your cancer journey—from understanding cancer types to mastering precision oncology.
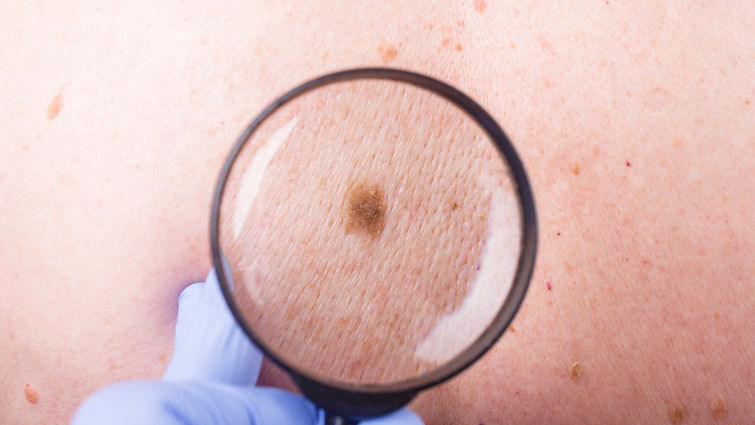
Sunbathing is commonly associated with relaxation, holidays, and achieving a tan. However, prolonged or repeated exposure to sunlight—especially without protection—can have serious long-term effects on skin health. One of the most well-established risks is the development of skin cancer. While moderate sunlight has benefits, excessive ultraviolet (UV) exposure is a major environmental factor linked to cancer formation.

Alcohol consumption is widely embedded in social culture across many parts of the world. While moderate drinking is often perceived as relatively harmless, growing scientific evidence suggests that long-term and excessive alcohol consumption is a significant risk factor for liver cancer, also known as hepatocellular carcinoma (HCC).
Understanding how alcohol affects the liver — often silently and over many years — is important for making more informed health decisions.
Vitamin C is an essential nutrient found in foods and supplements, and it plays important roles in collagen production, wound healing, and antioxidant function. In everyday nutrition, most people get enough vitamin C from food or standard supplements. But when people talk about high-dose vitamin C, they usually mean amounts far above normal dietary intake—especially doses given by intravenous (IV) infusion rather than by mouth. The National Cancer Institute notes that IV vitamin C can reach much higher blood levels than the same amount taken orally.
This distinction matters because oral vitamin C and IV vitamin C are not the same in practice. Oral doses are limited by how much the gut can absorb, while IV delivery can produce much higher blood concentrations. That difference is one reason high-dose vitamin C is often discussed in cancer-related research and complementary care, even though it is not the same as taking a routine over-the-counter supplement.
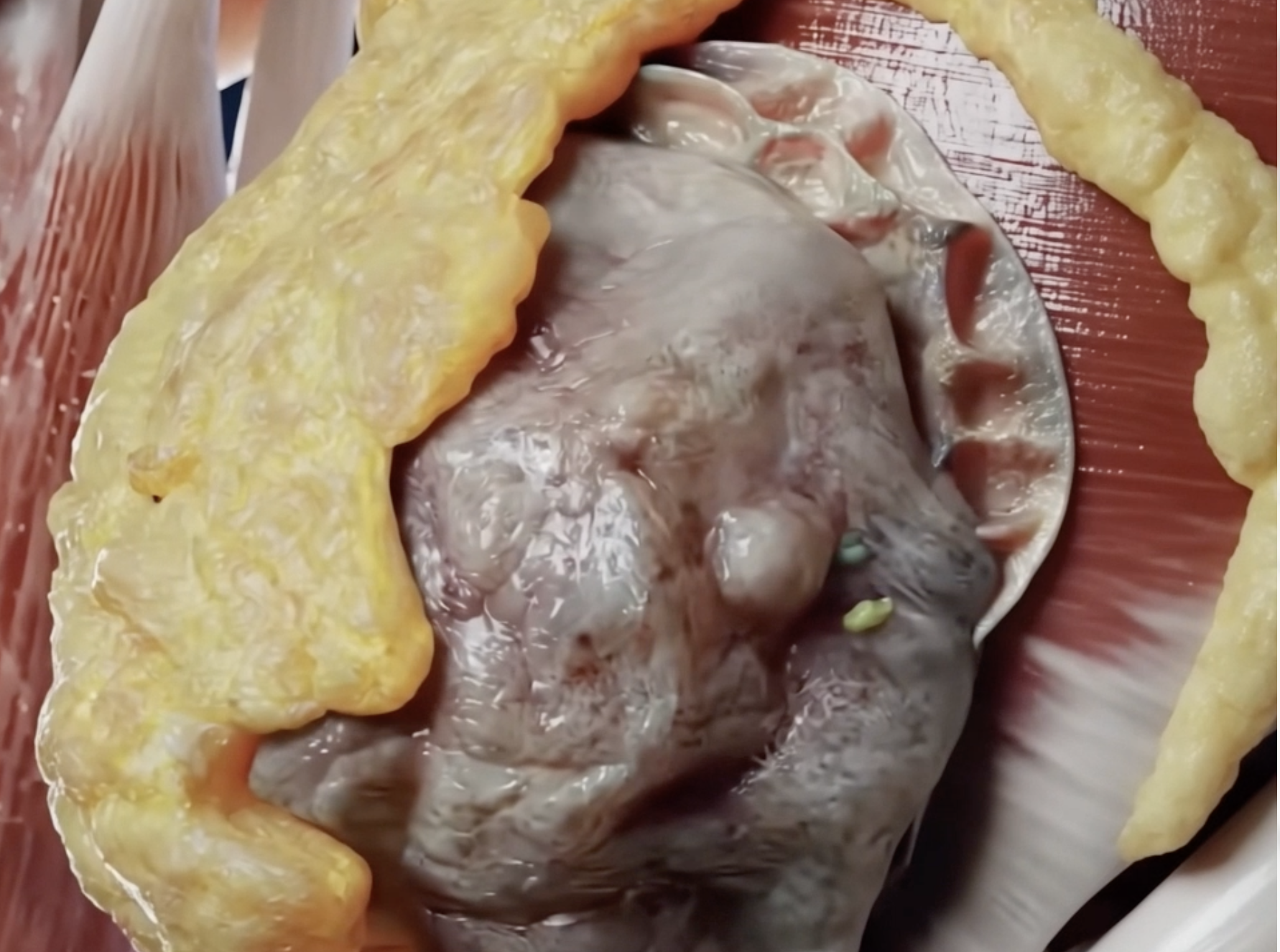
Breast cancer begins when cells in the breast start to grow in an abnormal and uncontrolled way. These cells can form a tumor and, over time, may invade nearby tissue or spread to other parts of the body. The National Cancer Institute notes that breast cancer is one of the most common cancers and that mammograms can sometimes detect it early, before it has spread.
Understanding how breast cancer develops can help patients and families make more sense of symptoms, screening, biopsy results, and the next steps in care. It can also explain why some breast cancers are found before symptoms appear, while others are only discovered after a lump or other visible change becomes noticeable.
One of the body’s natural defenses against cancer comes from a type of immune cell called the natural killer cell, or NK cell. NK cells are part of the innate immune system, which means they can respond quickly when they detect abnormal cells. The National Cancer Institute defines an NK cell as a type of white blood cell with granules containing enzymes that can kill tumor cells or virus-infected cells.
This matters because cancer cells are not just fast-growing cells. They are abnormal cells that may need to be recognized and removed before they continue growing or spreading. The immune system helps protect the body against disease, including some cancers, but cancer cells can sometimes avoid or suppress these defenses. Immunotherapy is built on this idea: helping the immune system find and attack cancer more effectively.
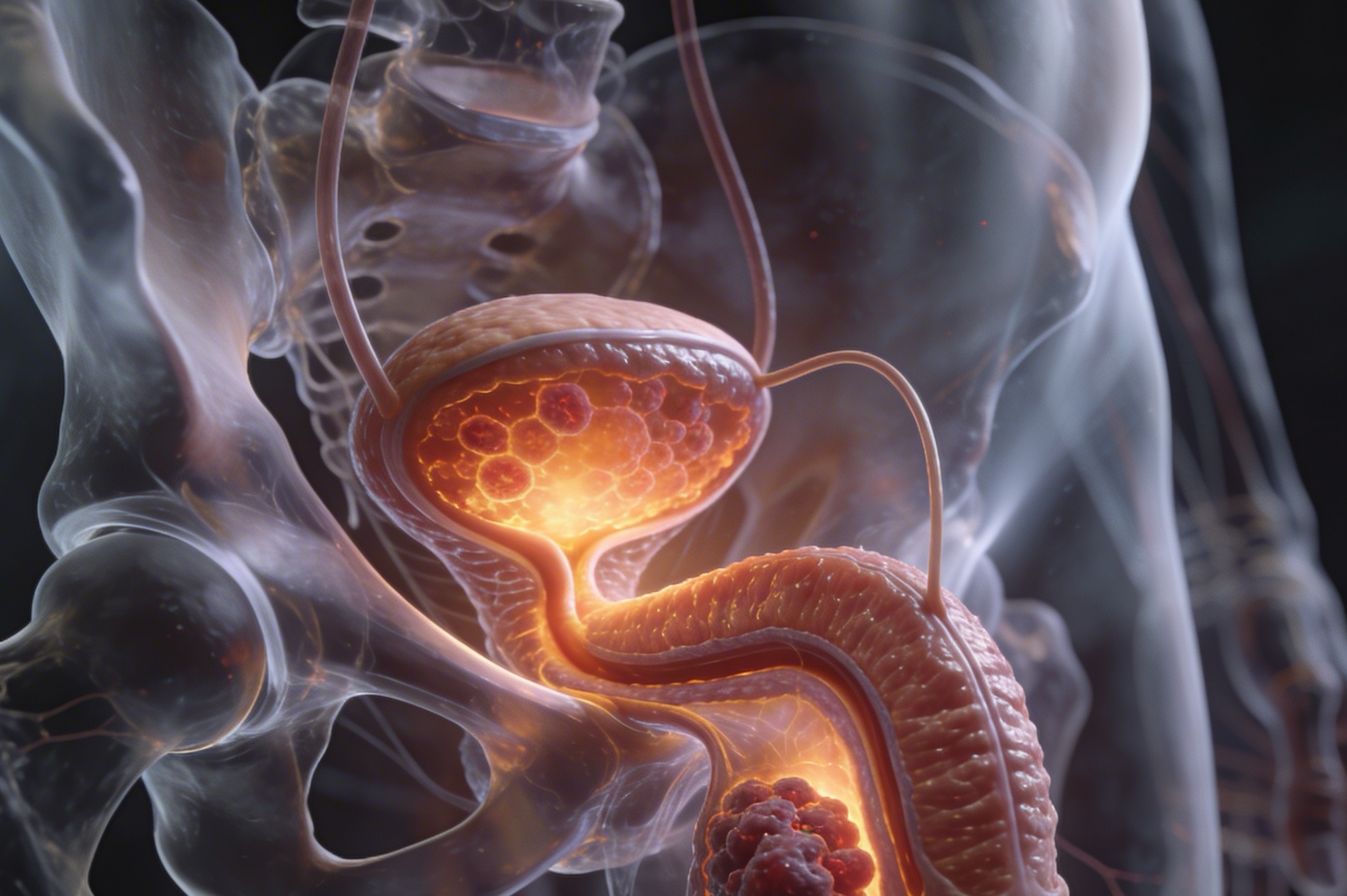
Prostate cancer begins when cells in the prostate start to grow in an abnormal and uncontrolled way. The prostate is a gland in the male reproductive system, and prostate cancer is one of the most common cancers affecting men. In many cases, it grows slowly, and some prostate cancers may not cause noticeable symptoms for a long time. That is one reason the condition can be difficult to recognize early without testing or screening discussions.
Understanding how prostate cancer develops can help patients and families make more sense of symptoms, risk factors, screening decisions, and next steps if further testing is needed. It can also help explain why some prostate cancers are found before symptoms appear, while others are discovered only after urinary or other changes become more noticeable
Cancer treatment is becoming more personalized, and one of the clearest examples of that shift is targeted therapy. Unlike traditional chemotherapy, which affects many fast-growing cells, targeted therapy is designed to act on specific changes in cancer cells that help them grow, divide, and spread. The National Cancer Institute defines targeted therapy as a type of cancer treatment that targets proteins or other molecules that cancer cells need to survive and spread.
This matters because not all cancers behave the same way. Even cancers that start in the same organ can have different mutations, proteins, or signaling pathways driving them. That is why targeted therapy is often considered part of precision medicine: it aims to match treatment to the biology of a person’s tumor rather than using the same drug for everyone.
For many patients, a tissue biopsy is one of the first important steps in understanding what may be happening inside the body. A tissue biopsy is a procedure that removes a small sample of tissue so it can be examined under a microscope or tested in the laboratory. While scans and blood tests can suggest that something is abnormal, a biopsy is often the test that helps doctors confirm what kind of cells are involved and whether cancer is present. The National Cancer Institute notes that a biopsy is often the only way to tell for sure if a person has cancer.
This matters because cancer care depends on understanding more than just where a mass is located. Doctors also need to know what kind of cells are involved and how those cells are behaving. The American Cancer Society explains that when doctors examine a section of tissue, they can see how the cells are arranged and, if cancer is present, how deeply a tumor may have grown. That kind of information helps move the discussion from suspicion to diagnosis.
Cancer can develop when changes occur in the DNA of cells. DNA contains the instructions that tell cells how to grow, divide, function, and repair themselves. When those instructions are changed in certain ways, the cell may begin behaving abnormally. The National Cancer Institute explains that cancer is caused by certain changes to genes that control the way cells function, especially how they grow and divide. The American Cancer Society similarly notes that cancer begins when some of the genes in a cell become abnormal, causing the cell to grow out of control.
These DNA changes are often called mutations or genetic changes. Not every mutation causes harm, and not every DNA change leads to cancer. In fact, cells are constantly finding and repairing many DNA mistakes. The National Human Genome Research Institute notes that mutations can happen as cells divide, but many are corrected by normal repair machinery. Cancer can develop when some of these changes affect key genes involved in cell growth, repair, or survival and are not successfully corrected.
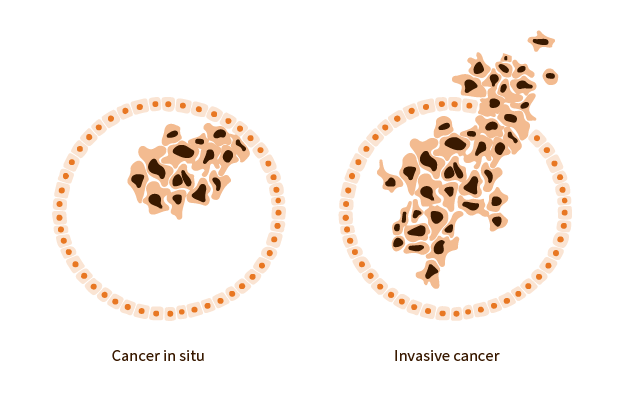
For many patients, one of the more confusing terms in a pathology report is “in situ.” In simple terms, in situ means “in its original place.” The National Cancer Institute explains that when abnormal cells are described as being “in situ,” they are found only in the place where they first formed and have not spread.
This matters because “in situ” often describes a very early form of abnormal cell growth. It may mean the cells look abnormal under the microscope, but they have not yet invaded nearby tissue. In many cases, this is why “in situ” is often associated with stage 0 disease.
For many patients, the words grade and stage can sound similar, but they do not mean the same thing. Tumor gradedescribes how abnormal cancer cells look under the microscope and can give doctors clues about how quickly the cancer is likely to grow or spread. The National Cancer Institute explains that low-grade cancer cells look more like normal cells and often grow more slowly, while high-grade cancer cells look more abnormal and may grow or spread faster.
Understanding tumor grade can make a pathology report easier to follow. It is one of the details doctors may use, along with stage, biomarkers, lymph node findings, and other test results, to understand the cancer more clearly and plan the next steps.
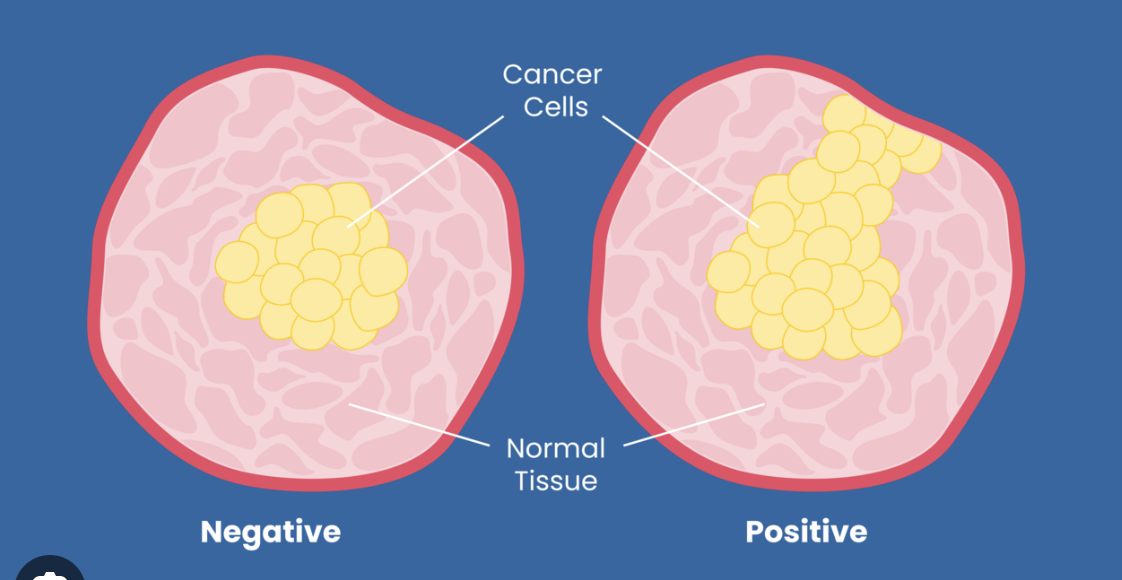
For many patients, one of the most confusing parts of a pathology report after surgery is the word “margins.” In cancer surgery, a margin is the edge or border of the tissue that was removed. When doctors say a margin is clear, clean, or negative, they mean no cancer cells were found at the edge of the removed tissue. When they say a margin is positive or involved, they mean cancer cells were found at the edge.
This matters because margins help doctors understand whether the tumor appears to have been fully removed from that area. A clear margin usually suggests that no cancer cells were seen at the outer edge of the specimen, while a positive margin suggests that cancer cells may still have been left behind in the body.

For many patients, one of the most important documents in cancer care is the pathology report. This is the report created after a pathologist examines tissue, cells, or fluid taken during a biopsy or surgery. It is often the document that confirms whether cancer is present and, if it is, provides some of the most important details about what kind of cancer it is. The National Cancer Institute explains that pathology reports describe what was found in the tissue sample and may include the diagnosis, tumor grade, tumor size, lymph node status, margin status, stage, and biomarker or molecular test results, depending on the case.
Because pathology reports contain medical language, they can feel intimidating to read. But understanding the basic purpose of the report can make the next steps feel clearer. A pathology report is not just paperwork. It is one of the main tools doctors use to understand the biology of a cancer and plan treatment.
For many people, one of the most worrying words they hear in cancer care is metastasis. Metastasis is when cancer spreads from the place where it first formed to another part of the body. In metastasis, cancer cells break away from the original tumor, travel through the blood or lymph system, and form new tumors in other organs or tissues. Even though the cancer has spread, the metastatic tumor is still made of the same type of cancer cells as the original tumor.
What many people do not realize is that this process may begin before scans can clearly detect it. Very small numbers of cancer cells can sometimes spread from the primary tumor and remain too few to be picked up by standard screening or diagnostic tests. The National Cancer Institute defines micrometastasis as small numbers of cancer cells that have spread from the primary tumor to other parts of the body and are too few to be picked up in a screening or diagnostic test.
For many people, one of the first new terms they hear after a cancer diagnosis is staging. Cancer staging is the process doctors use to describe how much cancer is in the body, how large it is, and whether it has spread. This information is important because it helps the care team understand the extent of the disease and plan the most appropriate next steps. The National Cancer Institute defines staging as performing exams and tests to learn the extent of cancer in the body, especially whether it has spread from where it first formed to other parts of the body.
Understanding stage can make a diagnosis feel slightly less overwhelming. It gives patients and families a clearer picture of what doctors have found and why certain tests or treatments are being recommended. The American Cancer Society notes that staging helps doctors determine the best treatment options and use survival statistics more meaningfully.
Cancer treatment is becoming more personalized, and one of the clearest examples of that shift is targeted therapy. Unlike traditional chemotherapy, which affects many fast-growing cells throughout the body, targeted therapy is designed to act on specific features inside or on cancer cells that help them grow, divide, and survive. The National Cancer Institute defines targeted therapy as a type of cancer treatment that targets the changes in cancer cells that help them grow, divide, and spread.
This matters because cancer is not one single disease. Even cancers that start in the same organ can behave very differently depending on their genes, proteins, and molecular signals. Targeted therapy is part of precision medicine, which aims to match treatment to the biology of a person’s tumor rather than using the same approach for everyone. Biomarker testing is one of the main tools doctors use to decide whether a targeted therapy may be appropriate.
Hearing the word “tumor” can be frightening, but not every tumor is cancer. A tumor is an abnormal mass of tissue that forms when cells grow and divide more than they should or do not die when they should. Tumors can be benign, meaning noncancerous, or malignant, meaning cancerous. Understanding the difference between benign and malignant tumors can help patients and families make sense of test results, imaging findings, and biopsy reports.
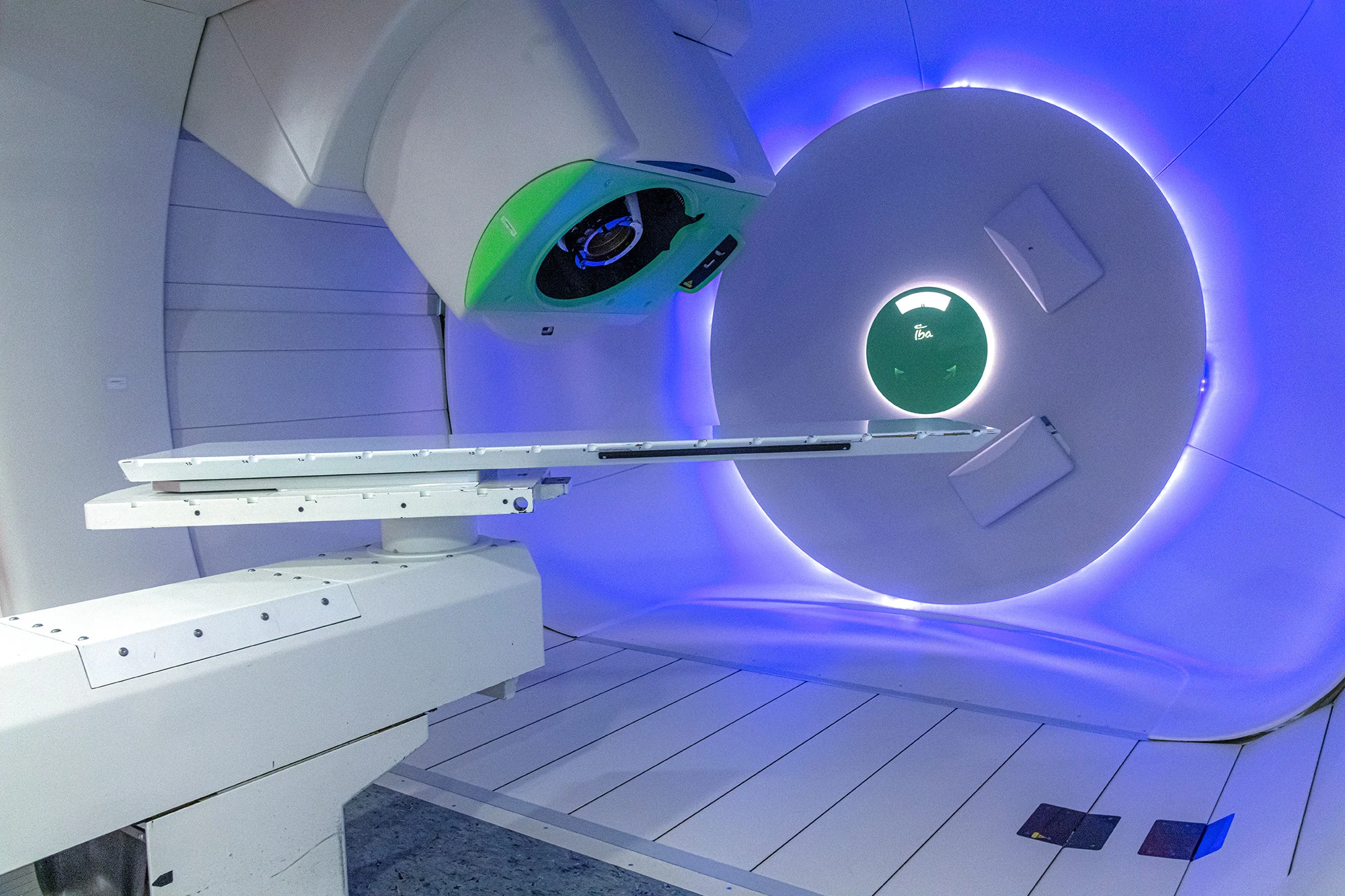
For many people diagnosed with cancer, hearing the word “radiation” can feel overwhelming. But radiation therapy is not just one treatment. There are different ways radiation can be delivered, and one of the more advanced forms is proton therapy. Proton therapy is a type of radiation treatment that uses protons, which are positively charged particles, to damage or destroy tumor cells. Unlike standard X-ray radiation, proton beams can be controlled so that most of their energy is released at the tumor, which may reduce radiation exposure to nearby healthy tissue.
This difference is what makes proton therapy especially important in situations where a tumor is close to sensitive structures such as the brain, eye, spine, or other critical organs. It has also become an important option in some childhood cancers, where reducing radiation to developing tissues can matter greatly. At the same time, proton therapy is not the right choice for every patient or every cancer, and researchers are still studying when it offers the clearest advantage over traditional radiation.
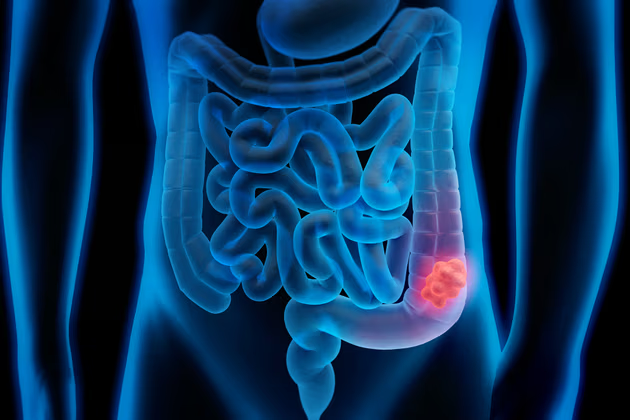
What starts as a small growth in the colon or rectum can sometimes become something far more serious over time. Colorectal cancer often develops slowly, usually beginning as a polyp — an abnormal growth in the lining of the colon or rectum. In many cases, these early changes do not cause symptoms, which is one reason colorectal cancer can go unnoticed until it becomes more advanced. Understanding how colorectal cancer develops helps explain why screening, symptom awareness, and early attention matter so much.

What starts as a small, painless change on the tongue can sometimes become something far more serious over time. Tongue cancer may begin with abnormal cells that grow quietly, without causing obvious discomfort in the early stages. Because the mouth can change for many reasons — including irritation, ulcers, or infection — early warning signs are sometimes overlooked or mistaken for something less serious. By the time changes become more noticeable, the disease may already be more advanced. Understanding how tongue cancer develops helps explain why awareness and early attention matter so much.

For decades, cancer treatment focused mainly on directly removing or destroying tumor cells through surgery, chemotherapy, or radiation therapy. While these approaches remain important, newer treatment strategies have changed the cancer care landscape in significant ways. One of the most important advances is immunotherapy.
Unlike traditional treatments that attack cancer directly, immunotherapy works by helping the body’s own immune system recognize and fight cancer cells. This has led to remarkable results for some patients, including long-term responses in certain cancers. At the same time, immunotherapy does not work for everyone, and the reasons are often linked to the complex biology of each person’s cancer.
Understanding how immunotherapy works—and why some patients respond while others do not—can help patients and families make more informed decisions about treatment options.
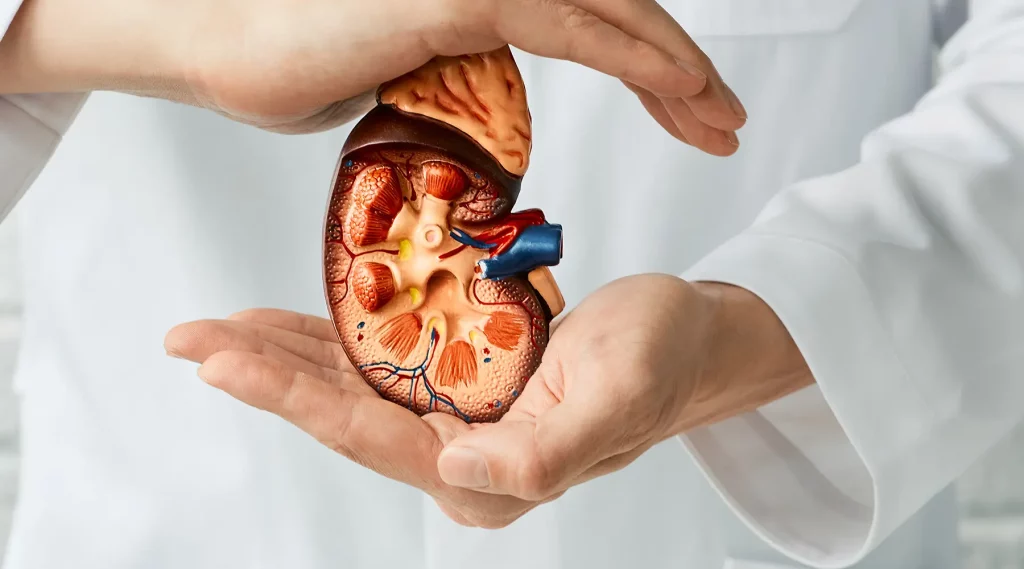
Kidney cancer is often described as a “silent” disease—and for many patients, that description is alarmingly accurate.
In fact, studies have shown that up to 50% of kidney tumors are discovered incidentally, meaning they are found during scans performed for unrelated reasons—such as back pain, abdominal discomfort, or routine health checks.

For many patients and families, cancer care involves more than scans and treatment schedules. Doctors may also talk about biomarkers, tumor markers, or biomarker testing to better understand the cancer and guide decisions. In simple terms, these tests look for certain genes, proteins, or other molecules that can provide clues about how a cancer behaves and which treatments may be more suitable.
Understanding these terms can make it easier to follow discussions about diagnosis, treatment planning, treatment response, and follow-up care. It also helps explain why modern oncology increasingly uses personalized or precision-based approaches instead of treating every cancer the same way.
For many people facing cancer, one of the most difficult and confusing moments is hearing that a treatment that once seemed effective is no longer working as expected. This can happen because cancer cells sometimes adapt over time, developing ways to survive treatment and continue growing. This process is known as drug resistance or treatment resistance.
Understanding why resistance happens can help patients and families make sense of treatment changes, additional testing, and new recommendations from their care team. It also helps explain why modern oncology increasingly relies on precision medicine and liquid biopsy to better understand how a cancer is changing and what treatment options may be most appropriate next.
For those facing melanoma—one of the most aggressive forms of skin cancer—immunotherapy has emerged as a life-changing treatment option. Among these breakthrough therapies, Opdivo (nivolumab) stands out for its ability to harness the body’s own immune system to fight cancer. But understanding how Opdivo works, who it’s right for, and what to expect during treatment can feel overwhelming. This guide breaks down the key details in clear, patient-centered language—empowering you to make informed decisions about your care.

The effectiveness of cancer treatment varies among each patient.