- +852 4750 3485
- info@mycancerinfo.org

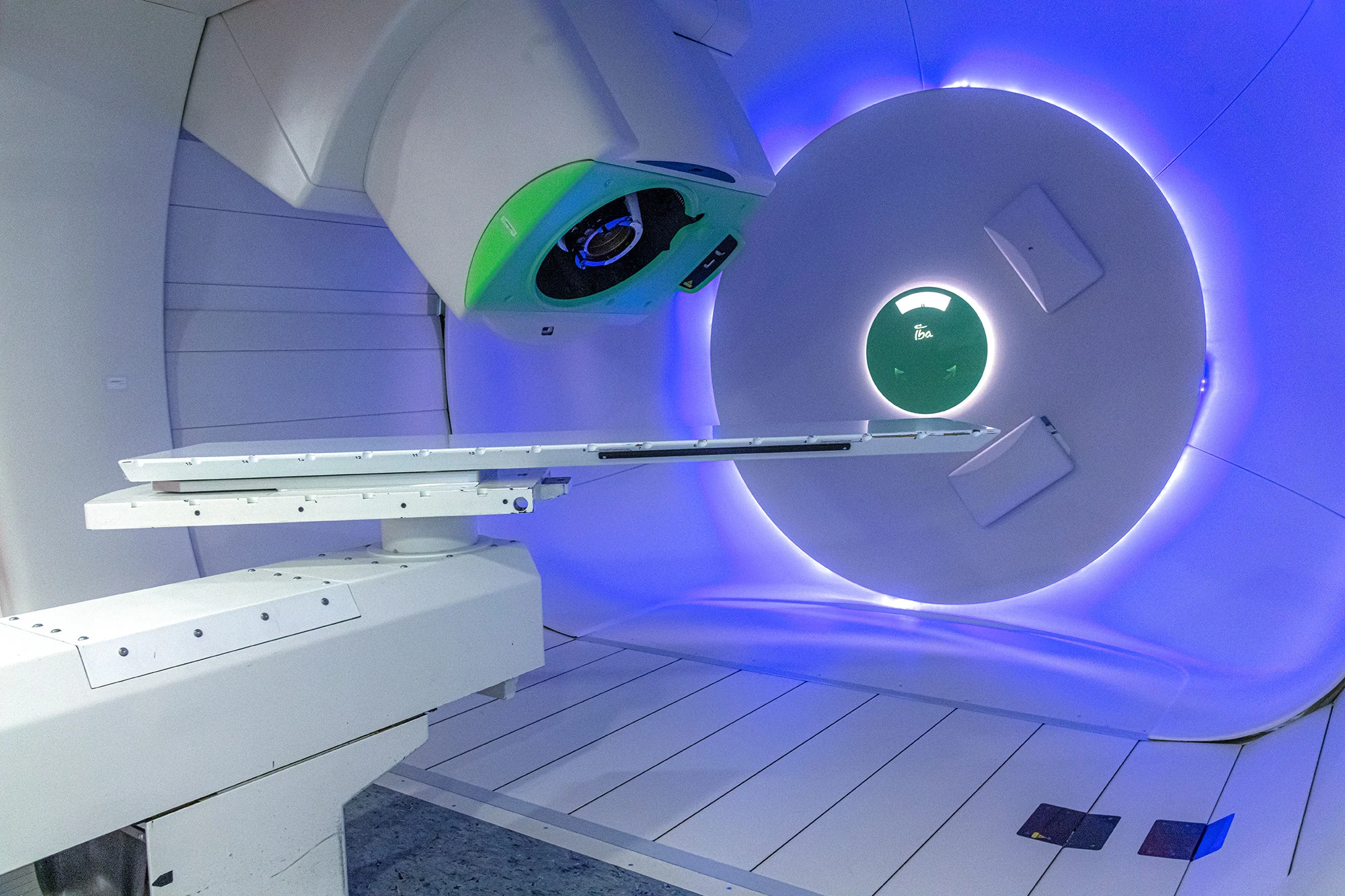
Proton therapy is a type of external beam radiation therapy. Like other forms of radiation, its goal is to damage the DNA of cancer cells so they cannot keep growing and dividing. The difference is in the type of energy used. Traditional radiation therapy uses X-rays, also called photons. Proton therapy uses streams of protons instead. Because proton beams can be aimed so that they stop at or near the tumor, they may deliver less radiation beyond the target area than standard X-ray treatment.
A simple way to think about it is this: traditional radiation often passes through the body and continues beyond the tumor, while proton therapy is designed to release most of its dose at the tumor and then stop. That added precision is why proton therapy is often discussed when doctors want to limit radiation exposure to nearby healthy tissue.
For proton therapy, special machines accelerate protons to very high energy and direct them toward the treatment area. Once the beam reaches the tumor, the protons deliver radiation that damages cancer cells. The American Cancer Society explains that the beam stops at the tumor instead of continuing beyond it, which is one reason proton therapy can sometimes lower the risk of side effects compared with traditional radiation.
This does not mean proton therapy causes no side effects at all. Some energy can still affect healthy tissues, and side effects depend on the body area being treated, the dose, and whether other treatments such as chemotherapy are also being used. But because the beam can be more tightly controlled, doctors often consider proton therapy when they want to protect structures close to the tumor as much as possible.
Proton therapy is sometimes used for tumors that are close to critical parts of the body or in cases where reducing radiation to surrounding tissue is especially important. Cancer organizations and major centers note it may be considered for some brain tumors, eye tumors such as eye melanoma, head and neck cancers, spine tumors, sarcomas near the skull base, lung cancer, liver cancer, prostate cancer, and certain childhood cancers. It may also be used in some noncancerous tumors or in selected cases when cancer comes back after prior X-ray radiation.
That said, proton therapy is not automatically better for every cancer. Mayo Clinic notes that few studies have directly compared proton radiation with X-ray radiation for many situations, and it is not yet clear that proton therapy improves survival across the board. In many cases, standard radiation remains the most appropriate choice.
Before treatment starts, patients usually go through a planning process called simulation. This often includes CT scans or MRI scans so the care team can map the exact treatment area and decide how to aim the proton beam. During this planning stage, the team also works out the best body position for treatment and may use cushions, restraints, or skin marks to help ensure the same positioning each time.
Treatment itself is usually given as an outpatient therapy, meaning most people do not stay overnight in the hospital. Many patients have sessions five days a week for several weeks, although the exact schedule depends on the cancer type and treatment plan. On treatment days, imaging such as X-rays or CT scans may be used to confirm the correct position before each session. The treatment is delivered by a machine, and the patient does not feel the radiation beam itself.
Most sessions involve time for setup, positioning, and imaging, even though the actual radiation delivery may take only a few minutes. Mayo Clinic notes that a full visit may take around 30 to 45 minutes including preparation, while the American Cancer Society notes that proton therapy sessions often last about 15 to 30 minutes including positioning and scans.
The main potential benefit of proton therapy is precision. Because the proton beam can stop at the tumor, there may be less radiation to normal tissue beyond the target. This may help reduce side effects, especially when treating tumors near important structures such as the brain, eyes, heart, spinal cord, or other sensitive organs. It may also allow doctors to give higher doses to the tumor in some cases.
Some evidence suggests proton therapy may reduce severe side effects compared with traditional radiation in certain settings. In an NCI-reviewed observational study of adults with advanced cancers treated with radiation and chemotherapy, patients who received proton therapy had fewer severe side effects requiring hospitalization than those who received traditional radiation, although survival outcomes were similar and the study had important limitations.
The effectiveness of cancer treatment varies among each patient.
Proton therapy also has limitations. It is more expensive than standard radiation, it is available only at a limited number of centers, and not all insurance plans cover it. The American Cancer Society and Mayo Clinic both note that proton therapy is not suitable for every cancer and that more research is still needed to define when it is clearly better than conventional radiation.
This is important for patients to understand. Proton therapy is a valuable tool, but it is still one option within a larger treatment plan. Whether it is appropriate depends on the type of cancer, the location of the tumor, prior treatments, overall health, and the goals of care.
Although proton therapy is designed to reduce unnecessary radiation exposure, side effects can still happen. Common side effects include fatigue, skin redness or irritation, soreness in the treated area, and hair loss in the part of the body being treated. Side effects usually depend on which body area is receiving radiation and often build up gradually over the course of treatment rather than appearing all at once.
Patients are often able to go home right after each session, and Mayo Clinic notes they do not become radioactive after treatment. Follow-up imaging may be recommended during or after therapy to see how the tumor is responding.
Proton therapy represents one of the more precise ways to deliver radiation for cancer treatment. For some patients, especially those with tumors near sensitive organs or certain childhood cancers, that precision may be an important advantage. But proton therapy is not a one-size-fits-all solution, and the best radiation approach depends on the individual patient and the specific cancer being treated.
As research continues, doctors are learning more about when proton therapy offers meaningful benefits and when other forms of radiation may work just as well. For patients, the most important question is not simply what is newest, but what is most appropriate for their own diagnosis, anatomy, and treatment goals.
At Cancer A-Z, you can request a 15 mins free-of-charge discussion with our cancer professionals.
National Cancer Institute. Definition of proton beam radiation therapy.
https://www.cancer.gov/publications/dictionaries/cancer-terms/def/proton-beam-radiation-therapy
American Cancer Society. Proton Therapy for Cancer.
https://www.cancer.org/cancer/managing-cancer/treatment-types/radiation/proton-therapy.html
Mayo Clinic. Proton therapy.
https://www.mayoclinic.org/tests-procedures/proton-therapy/about/pac-20384758
National Cancer Institute. Is Proton Therapy Safer than Traditional Radiation?
https://www.cancer.gov/news-events/cancer-currents-blog/2020/proton-therapy-safety-versus-traditional-radiation
Precision medicine provides patients with clearer and more personalized treatment guidelines


Learn how precision medicine can help with your cancer treatment

The effectiveness of cancer treatment varies among each patient.